What Is Articular Cartilage?
Articular cartilage is a white smooth connective tissue that lines the bony surfaces of joints.
Hyaline Cartilage
Articular cartilage is a type of cartilage known as hyaline cartilage. Hyaline cartilage is often described as glass-like in appearance due to its semi-translucent pearl grey color. The goal of cartilage restoration procedures is to encourage the new growth of hyaline cartilage.
Synovial Joint
The most common type of joint is called a synovial joint and is capable of much articulation. Synovial joints include the knee, elbow, hip, ankle, and wrist. Articular cartilage is a living tissue with no blood vessels or nerves covering the ends of bones where they meet to form joints. It provides a smooth, lubricated surface that acts as a shock absorber and allows the joint to articulate and withstand weight-bearing movements for daily activities and athletics, including stair climbing and work-related activities.
Limited Healing Capabilities
One of the key issues with articular cartilage is it has a limited capacity for intrinsic healing and repair. In essence, it cannot heal on its own, which is a problem as it is subject to a significant amount of wear and tear. Due to the unique and complex structure of articular cartilage, treatment and repair of any damage is challenging. Our expert orthopedic surgeons and physical therapists at AICA Orthopedics Tucker are exceptionally familiar with treatment options for damaged articular cartilage. Please contact us to start your journey to healing today!
Cartilage Damage
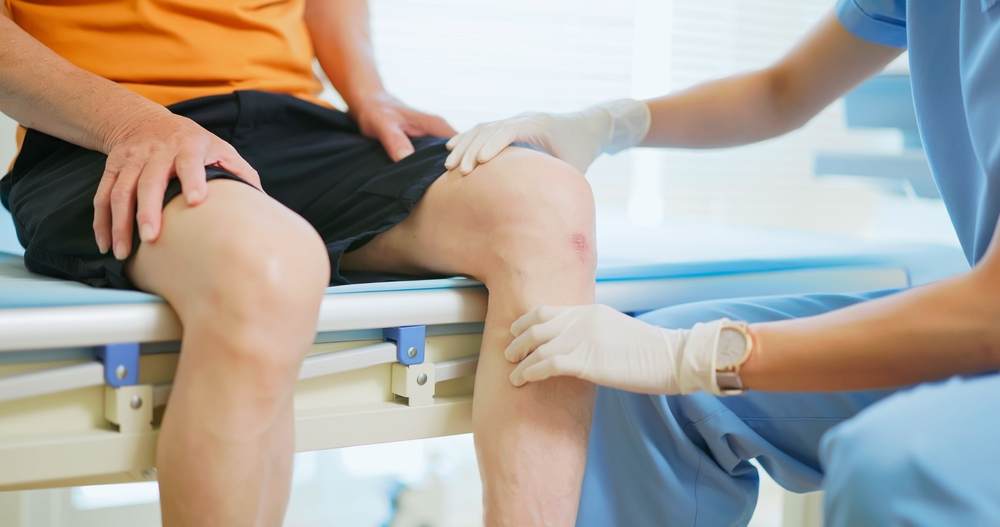 Articular cartilage injuries most frequently occur in the knee, but they may also involve the hip, ankle, shoulder, and ankle. While some articular cartilage injuries do not cause any symptoms, it is more common for a person to experience a range of possible symptoms.
Articular cartilage injuries most frequently occur in the knee, but they may also involve the hip, ankle, shoulder, and ankle. While some articular cartilage injuries do not cause any symptoms, it is more common for a person to experience a range of possible symptoms.
Symptoms
While symptoms vary from patient to patient, the following are some common symptoms to watch for. If you experience any of these, please contact AICA Tucker to set up an evaluation by our expert physicians.
- Knee swelling
- Joint pain
- A ‘locking’ or ‘catching’ feeling
- Stiffness and decreased range of motion
- The feeling of the joint being unstable
- Crackling or grating when bending the joint
Identifying Damage
If you are experiencing pain, joint stiffness, or any of the other symptoms mentioned above, please contact AICA to schedule an evaluation. Our physicians will evaluate you for signs of articular cartilage damage. The following imaging might be utilized.
X-Ray and MRI
An X-ray or MRI (magnetic resonance image) study may be used to identify any damage and the severity. These imaging studies help our doctors to detect any damage to the articular cartilage, underlying bones, and surrounding ligaments and tissues. If you have arthritis, weight-bearing x-rays will show bone touching bone due to the extensive cartilage loss.
Arthroscopy
A procedure known as arthroscopy is done to more thoroughly diagnose articular cartilage damage or injury. Arthroscopy is a minimally invasive surgical procedure involving one to three small incisions around the affected joint, inserting a small tube camera, the arthroscope, and surgical tools into the joint. The camera transmits a video of the inside of the joint to a monitor, allowing the surgeon to see the structures and tissues of the joint up close. Being able to see the structures with more than imaging studies can allow for better diagnosis and a stronger surgical plan.
How Does Articular Cartilage Damage Occur?
 Due to the nature of articular cartilage not being able to repair or heal itself well, doctors have developed several techniques to stimulate the growth of new cartilage and repair damaged cartilage. Articular cartilage can be damaged by normal wear and tear or by injury. Treating damaged articular cartilage can relieve pain and ease movement, but one of the biggest benefits is preventing arthritis.
Due to the nature of articular cartilage not being able to repair or heal itself well, doctors have developed several techniques to stimulate the growth of new cartilage and repair damaged cartilage. Articular cartilage can be damaged by normal wear and tear or by injury. Treating damaged articular cartilage can relieve pain and ease movement, but one of the biggest benefits is preventing arthritis.
Direct Trauma
A forceful impact during sports or from a fall can damage the articular cartilage. Due to no blood supply in the cartilage, it is often unable to repair itself. Occasionally if the damage is more severe and penetrates the bone, the underlying bone will provide blood to the area and potentially help with the repair.
Progressive Degradation
Normal wear and tear of articular cartilage occur with the progressive loss of cartilage through no direct trauma. Aging and participating in activities that require overuse of your joints put repetitive wear on the cartilage cushioning your joints. As the articular cartilage wears down, it softens and then fragments, exposing the bone below.
Cartilage Fragments
Occasionally, trauma to the joint can result in a cartilage fragment breaking loose from the bone and floating in the joint. This chip, or loose body, can interfere with normal joint motion and is often the cause of the “locking feeling” in a joint.
What Makes a Good Candidate?
Ideally, a candidate for cartilage repair is someone under 50 with a relatively healthy knee with no (or limited) arthritis. More specifically, the ideal patient is between 18 and 35 with one specific injury or lesion.
While cartilage repairs can be performed on people of all ages, patients over 50 or with significant defects to the cartilage will not see the same benefits as the ideal candidate. Studies have shown that cartilage repairs are slow, and the maturation of the repair continues even four years post-op.
Common Repairs for Articular Cartilage Damage
Microfracture
The goal of microfracture is to stimulate the growth of new articular cartilage. This is achieved by creating a new blood supply by routing new cells to the surface of the joint. The surgeon will use a sharp tool called an awl to drill small holes in the bone into the subchondral bone and bone marrow underneath the damaged articular cartilage. Similar to a fracture, these holes stimulate the bone marrow to repair the damage.
The new cartilage formed from this healing response is not articular cartilage. It is fibrocartilage commonly found in intervertebral discs and ligaments. While it can keep the bones of a joint from rubbing against each other, it is not as durable as normal, healthy articular cartilage.
Drilling
Drilling is an articular cartilage reconstruction similar to microfracture. Like microfracture, drilling stimulates the production of healthy cartilage by drilling holes in the bone. Using a surgical drill or wire, multiple holes are made through the injured area into the subchondral bone. This penetration stimulates a healing response. Drilling can be done with an arthroscopy, but it is less precise than microfracture. The drill can also heat up too much and damage some of the surrounding tissues.
Abrasion Arthroplasty
Also done with an arthroscope, abrasion arthroplasty utilizing high-speed burrs removes the damaged cartilage to reach the subchondral bone.
Autologous Chondrocyte Implantation (ACI)
An autologous chondrocyte implantation (ACI) is a two-step procedure and cannot be done completely with an arthroscope. During the first procedure, a surgeon arthroscopically removes healthy articular cartilage from part of the non-weight bearing joint.
This tissue is sent to a laboratory where chondrocytes (a type of cartilage cell and where the name of the procedure comes from) are harvested and grown over the course of several (3-5) weeks.
At the end of 3-5 weeks, the cultivated cells are taken and implanted into the site of damaged articular cartilage. This procedure is an open procedure (arthrotomy) and cannot be done arthroscopically.
To secure the new cells to the damaged site a layer of periosteum, bone lining tissue is sewn over the area. This cover is then sealed with fibrin glue. More of the healthy cultivated cells are injected into the defect under the patch.
This procedure is a popular procedure for younger patients with single, large defects. One of the advantages of an ACI is the implanted cells are cultivated from the patient, so rejection isn’t a possibility. On the other hand, an ACI is a two-step procedure that takes several weeks to complete in addition to a longer recovery due to it being an open procedure.
Whole Tissue Procedures
Osteochondral Autograft Transplantation – Patient Tissue
During osteochondral autograft transplantation, a surgeon utilizes plugs of healthy articular cartilage and subchondral bone and transplants them from one area over a joint to the injured area of the joint.
The plug of healthy cartilage, the graft, is removed from a non-weight-bearing part of the joint and inserted into a small hole made by a drill. This can be done once or several times by inserting healthy plugs into several different holes in the damaged area. If multiple plugs are transferred, this is called a mosaicplasty.
The inserted plugs restore the smooth surface of the articular cartilage allowing the joint to move smoothly and without pain.
There are limits to this procedure when done in the knee because there are only a few non-weight-bearing areas in the knee from which plugs can be taken, so this procedure is normally utilized for small defects. If it is a small defect, this can be done arthroscopically but can also be done as an open procedure.
Osteochondral Allograft Transplantation – Cadaver Tissue
The osteochondral allograft transplantation is very similar to the osteochondral autograft described above but uses tissue from a cadaver instead of from the patient.
A surgeon will typically opt for an osteochondral allograft for large areas of articular cartilage restoration and can be shaped to fit the exact dimensions of the defect. Because the surgeon is taking the graft from a cadaver, there is no compromising the patient’s existing non-weight-bearing tissues.
Due to the cartilage and bone coming from a donor, there is a possibility of rejection. The other consideration is the transplanted cartilage might not be as durable as the patient’s own. Osteochondral allografts are done via an open procedure due to the large graft.
Stem Cells and Tissue Engineering
Tissue engineering is research focused on new ways to make the body grow healthy cartilage tissues. The current theory is to use growth factors to stimulate new tissue that may be isolated, transplanted, and used to induce new cartilage formation.
Mesenchymal stem cells are currently being tested in a similar method. Instead of growth factors, researchers are taking mesenchymal stem cells obtained from human tissue, such as bone marrow, and placing them in a specific environment with the hypothesis that they can develop into, and give rise to, cells similar to the host tissue.
While the research and ideas are promising, tissue engineering procedures are still at an experimental stage. These procedures are not commonly done in orthopedics centers but are being tested in labs and clinical trials.
Rehab
Physical Therapy
 Most patients will be non-weight bearing for the first two to three weeks following articular cartilage restoration surgeries. Utilizing crutches to maintain some mobility. You will start physical therapy approximately one week after surgery on an outpatient basis.
Most patients will be non-weight bearing for the first two to three weeks following articular cartilage restoration surgeries. Utilizing crutches to maintain some mobility. You will start physical therapy approximately one week after surgery on an outpatient basis.
Other than rest and time, physical therapy is a vital part of your recovery process. Your team of surgeons and physical therapists will develop a plan to strengthen and stabilize the joint as well as surrounding muscles and ligaments.
The goal of physical therapy is to help restore mobility to the affected joints, which will typically be outpatient and monitored by both your physical therapist and surgeon. Post-operative MRIs may also be required to monitor the progress.
After surgery, even once you are weight-bearing, it is important to protect the surface where either graft or cells have been implanted. This might require wearing a brace, just being aware of your surroundings, and taking it easy.
Recovery Time
As long as you are maintaining your physical therapy protocol, it is possible to return to your normal level of daily activity approximately four to six weeks after surgery. Clearance for sports will take longer, with an average of 6 months post-op. High-impact sports may take longer to return to full participation.
Of course, each procedure has a variable timetable for a return to daily activities, work, and sports. Our expert orthopedic surgeons, sports medicine physicians, and physical therapists at AICA Orthopedics Tucker will work with you to determine the most likely timetable to get you back on your feet.
